Dental Restorations Part 3: Amalgam
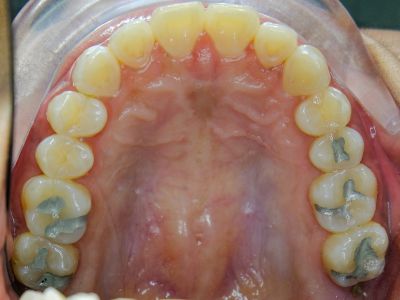
In previous generations, direct, done-in-the-mouth restorations were only possible with amalgam or a gold foil These single-appointment options could provide very long-term function and durability. An amalgam is made of metals such as mercury, tin, silver, and copper, and has been used in dentistry for more than 170 years.
Amalgams began in a time when there was a need for a material that could restore teeth conveniently, predictably, and remain working. A dentist may not have been easily accessible either! As one of the most original restorations, this design proved to be so successful that it continues in use today, with several advantages that remain superior.
Amalgam restorations do not require meticulous conditions to be placed and continue working; they can be delivered in the presence of saliva, and are retained mechanically in the tooth — which means as long as the tooth and the filling are intact, the amalgam stays in place. An amalgam is resistant to acid from sources such as plaque, beverages (soda, citrus drinks), and food (tomatoes, fruits, etc), and can survive in circumstances that would challenge comparable tooth-colored composites. By its metallic nature, amalgam has antimicrobial properties, so it is additionally difficult for plaque to compromise it. In fact, for patients with a high risk for cavities and continued plaque challenges, these fillings are steadfast in their ability to perform.
In dentistry, there is a phenomenon called microleakage. This refers to the migration of fluid and bacteria between a restoration and the tooth it is connected to. The closer the fit, the less the leakage. This applies to all restorations, and occurs in different degrees based on the material chosen. Microleakage can lead to increased tooth sensitivity, the failure of a restoration, a cavity, or even a root canal if bacteria compromise the nerve. As a result, a restoration must seal the tooth from the outside environment as much as possible. Without any other complication, this is ultimately what will cause any restoration to fail with time.
When it comes to amalgam, the material corrodes into the tooth to form an incredible natural seal. As the years go on, this seal does deteriorate, causing the need for replacement – however that can occur after decades. With tooth-colored composites, bonding can be compromised faster, sometimes after only several years.
Amalgam has some drawbacks. It may produce a small electric sensation if it contacts other metals, it may require more tooth structure to be removed for placement, and it can also permanently stain some of the tooth or tissue it touches – so placement in the back of the mouth is more desirable.
Of particular interest, an amalgam is made of about 50% mercury. Notice I did not say this is necessarily a drawback, as mercury is the only metal in existence that allows this restoration to succeed and help people in the ways it does. Mercury has led to much health concern over the past several decades. So how can mercury in amalgam be better understood? Studies do show there are higher levels of mercury in the bodies of people with amalgam restorations. The question of debate was whether or not this amount is significant. Massive international research studies took place over the last 50 years in efforts to find health hazards from this material. And they were repeated, and repeated. After all these attempts, no credible (key word, credible) evidence was found showing a significant association between amalgam restorations and disease. Verified effects were allergic or hypersensitivity reactions. In fact, after the last enormous research undertaking which concluded in 2010, the decision was made to cease further efforts to find problems with this material. Amalgam is approved for use by the FDA, and the exceptional groups that may be at greater risk for health effects include women who are nursing or plan to become pregnant, unborn children, children under age 6, people with metal allergies, impaired kidney or liver function, or neurological disease.
To relate the amount of mercury someone can be exposed to, a publication I like to reference is called “Estimation by a 24-hour Study of the Daily Dose of Intra-oral Mercury Vapor Inhaled after Release from Dental Amalgam” by Anders Berglund in 1990, who found that the daily mercury exposure from patients with at least nine amalgam restorations in their mouth was 1% of the World Health Organization’s maximum daily amount of mercury exposure an employee could receive in the workplace at the time. It is worth noting that this is not the only study on the subject, and the amount released can vary by personal habits such as grinding and brushing. Regardless, the rationale behind this small release is due to the understanding that mercury and the other metals in an amalgam react with one other to form a stable compound, and the majority of mercury becomes locked in the material after placement.
Mercury in amalgam is actually released primarily during placement or removal, because this is when the amalgam is drastically altered. In fact, the main way mercury from amalgam is ingested is not through swallowing, but through inhalation. Eating tuna will get you more mercury! Don’t believe me? Think of it this way: if the mercury in an amalgam was being released and continuously bathing the body, a lot of this restoration would evaporate out of the tooth – and that would be quite noticeable. Amalgam restorations in service after decades still retain almost all of their shape. This difference? A very small or indiscernible amount of lost ingredients, including mercury, and the other metals. Environmental accumulation of mercury is also important, so to help keep the environment safe, many dental practices are now required to have filters to separate mercury from general waste. What more, amalgams use a lot less plastic to provide than tooth-colored composites, which also accumulates in the environment.
To attest to the durability of these restorations, when I was a resident treating veterans at the VA, it was not uncommon to see a 40 year old filling still performing healthily in the tooth - some made under a tent during a foreign campaign!. When amalgams are also discussed, some claim these fillings cause an increased risk of cracks or tooth fracture. I would say by all reasonable assessments that this risk exists for any filling in a tooth. Amalgams can expand anywhere from 0.1-1%, and tooth-colored composites contract around 0.1-5% and get fractures or cracks as well. If the tooth fractures or gets a crack, it was either because the filling was big and less natural tooth remained, or because the filling lasted so long it outperformed the tooth which began cracking around it. Amalgams also can cause less tooth sensitivity because there are no adhesive chemicals in them or used during placement, unlike tooth-colored composites.
Ultimately, most fillings will need replacement and lead to crowns. There is nothing that is as good as natural tooth structure, and it should be conserved if possible. So a cost benefit analysis should be made. Is there mercury in an amalgam? Yes. Is this a cause for concern? I would use them in my own teeth and those of my family. With shorter-lasting fillings, more time, money, and retreatment will be needed, and teeth will likely need crowns sooner - risking other problems that can follow, such as root canals, extractions, or implants. So the longer a filling can last, the better off someone will be. Amalgam restorations are durable, affordable, and have the potential to last very long amounts of time. They remain a well-studied and extremely effective restoration this day.
